 Description
Description - Appendicitis is inflammation of the appendix.
- When the appendix becomes inflamed or infected, rupture may occur within a matter of hours, leading to peritonitis and sepsis.
Risk Factors
- Obstruction by fecalith or foreign bodies, bacteria or toxins.
- Low-fiber diet
- High intake of refined carbohydrates
Signs and Symptoms/ Assessment
- Pain in the periumbilical area that descends to the right lower quadrant.
- Abdominal pain that is most intense at McBurney’s point
- Rebound tenderness and abdominal rigidity
- Low-grade fever
- Elevated white blood cell count
- Anorexia, nausea, and vomiting
- Client in side-lying position, with abdominal guarding and legs flexed
- Constipation or diarrhea
Diagnostic Evaluation
- Diagnosis is based on a complete physical examination and laboratory and radiologic tests.
- Leukocyte count greater than 10,000/mm 3, neutrophil count greater than 75%; abdominal radiographs, ultrasound studies, and CT scans may reveal right lower quadrant density or localized distention of the bowel.
Primary Nursing Diagnosis
Primary Preoperative Nursing Diagnosis
- Pain (acute) related to inflammation
- Risk for infection related to the surgical incision
Other Diagnoses that may occur in Nursing Care Plans For Appendicitis
- Imbalanced nutrition: Less than body requirements
- Impaired skin integrity
- Ineffective tissue perfusion: GI
- Risk for deficient fluid volume
- Risk for injury
Medical Management
An
appendectomy (surgical removal of the appendix) is the preferred method of
management for acute appendicitis if the inflammation
is localized. An open appendectomy is completed with
a transverse right lower quadrant incision, usually
at the McBurney point. A laparoscopic appendectomy may be used in females of
childbearing age, those in whom the diagnosis is in
question, and for obese patients. If the appendix has ruptured
and there is evidence of peritonitis or an abscess, conservative treatment
consisting of antibiotics and intravenous (IV) fluids is given 6 to 8 hours prior to an appendectomy.
Generally, an appendectomy is performed within 24 to 48 hours after the onset
of symptoms under either general or spinal anesthesia. Preoperative
management includes IV hydration, antipyretics, antibiotics, and, after
definitive diagnosis, analgesics.
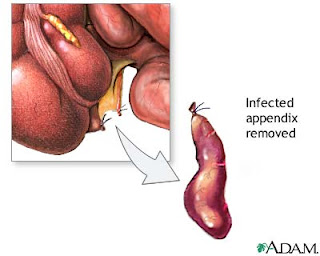
Appendectomy (surgical removal of the appendix)
Complications of Appendectomy
- The major complication is perforation of the appendix, which can lead to peritonitis or an abscess.
- Perforation generally occurs 24 hours after onset of pain, symptoms include fever (37.7°C [100° F] or greater), toxic appearance, and continued pain and tenderness.
Pharmacologic Intervention
- Crystalloid intravenous fluids an isotonic solutions such as normal saline solution or lactated Ringer’s solution 100–500 mL/hr of IV, depending on volume state of the patient, is used to replaces fluids and electrolytes lost through fever and vomiting; replacement continues until urine output is 1 cc/kg of body weight and electrolytes are replaced
- Antibiotics (broad-spectrum antibiotic coverage) to control local and systemic infection and reduces the incidence of postoperative wound infection
- Other Drugs: Analgesics.
Nursing Intervention
Preoperative interventions
- Maintain NPO status.
- Administer fluids intravenously to prevent dehydration.
- Monitor for changes in level of pain.
- Monitor for signs of ruptured appendix and peritonitis
- Position right-side lying or low to semi fowler position to promote comfort.
- Monitor bowel sounds.
- Apply ice packs to abdomen every hour for 20-30 minutes as prescribed.
- Administer antibiotics as prescribed
- Avoid the application of heat in the abdomen.
- Avoid laxatives or enema.
- Monitor temperature for signs of infection.
- Assess incision for signs of infection such as redness, swelling and pain.
- Maintain NPO status until bowel function has returned.
- Advance diet gradually or as tolerated or as prescribed when bowel sound return.
- If ruptured of appendix occurred, expect a Penros drain to be inserted, or the incision maybe left to heal inside out.
- Expect that drainage from the Penros drain maybe profuse for the first 2 hours.
Documentation Guidelines
- Location, intensity, frequency, and duration of pain
- Response to pain medication, ice applications, and position changes
- Patient’s ability to ambulate and tolerate food
- Appearance of abdominal incision (color, temperature, intactness, drainage)
Discharge and Home Healthcare Guidelines
- MEDICATIONS. Be sure the patient understands any pain medication prescribed, including doses, route, action, and side effects. Make certain the patient understands that he or she should avoid operating a motor vehicle or heavy machinery while taking such medication.
- INCISION. Sutures are generally removed in the physician’s office in 5 to 7 days. Explain the need to keep the surgical wound clean and dry. Teach the patient to observe the wound and report to the physician any increased swelling, redness, drainage, odor, or separation of the wound edges. Also instruct the patient to notify the doctor if a fever develops. The patient needs to know these may be symptoms of wound infection. Explain that the patient should avoid heavy lifting and should question the physician about when lifting can be resumed.
- COMPLICATIONS. Instruct the patient that a possible complication of appendicitis is peritonitis. Discuss with the patient symptoms that indicate peritonitis, including sharp abdominal pains, fever, nausea and vomiting, and increased pulse and respiration. The patient must know to seek medical attention immediately should these symptoms occur.
- NUTRITION. Instruct the patient that diet can be advanced to her or his normal food pattern as long as no gastrointestinal distress is experienced.











0 comments:
Post a Comment